
Who Is a Good Candidate for Semaglutide? A Complete Guide
If you have been struggling to lose weight despite trying diet after diet, you are not alone. For many people in Franklin, TN, Nolensville, TN,

You finish breakfast, and before the last bite is swallowed, your mind is already planning lunch. You walk past a bakery and the smell hijacks your thoughts for the next hour. You ate enough to feel physically full, yet some part of your brain keeps whispering about snacks, meals, and everything in between.
If this sounds familiar, you are experiencing what researchers and patients now call “food noise.” It is not hunger. It is not a lack of willpower. It is a real, biological phenomenon that affects more than half of people living with overweight or obesity, a population that the CDC Adult Obesity Facts estimates at roughly 40% of U.S. adults. At Body Works in Franklin, TN and Nolensville, TN, we hear this story every day from patients researching medical weight loss. Here is the science behind food noise and how GLP-1 medications quiet it.
Food noise is the persistent, intrusive mental preoccupation with food that exists separate from physical hunger. Everyone thinks about meals sometimes. Food noise is different: it is constant, unwanted, and often distressing. A 2025 expert panel published in Nature defined it as “persistent thoughts about food that are perceived by the individual as being unwanted and/or dysphoric and may cause harm to the individual, including social, mental, or physical problems” (Nature, 2025).
Patients describe food noise as:

The critical distinction is that food noise is not hunger. Hunger is a physiological signal that your body needs fuel. Food noise is a cognitive phenomenon, a mental loop that continues even when your body has adequate energy. Reframing the struggle from a character flaw to a neurobiological condition is the first step toward treating it effectively.
Food noise starts with a brain system called the Default Mode Network, or DMN. Think of the DMN as your brain’s background setting, the network that activates when you are not focused on a specific task. It drives mind-wandering, daydreaming, and thinking about the future. Research published in PubMed Central found that our minds are in this wandering state roughly 47% of the time (PMC, 2024).
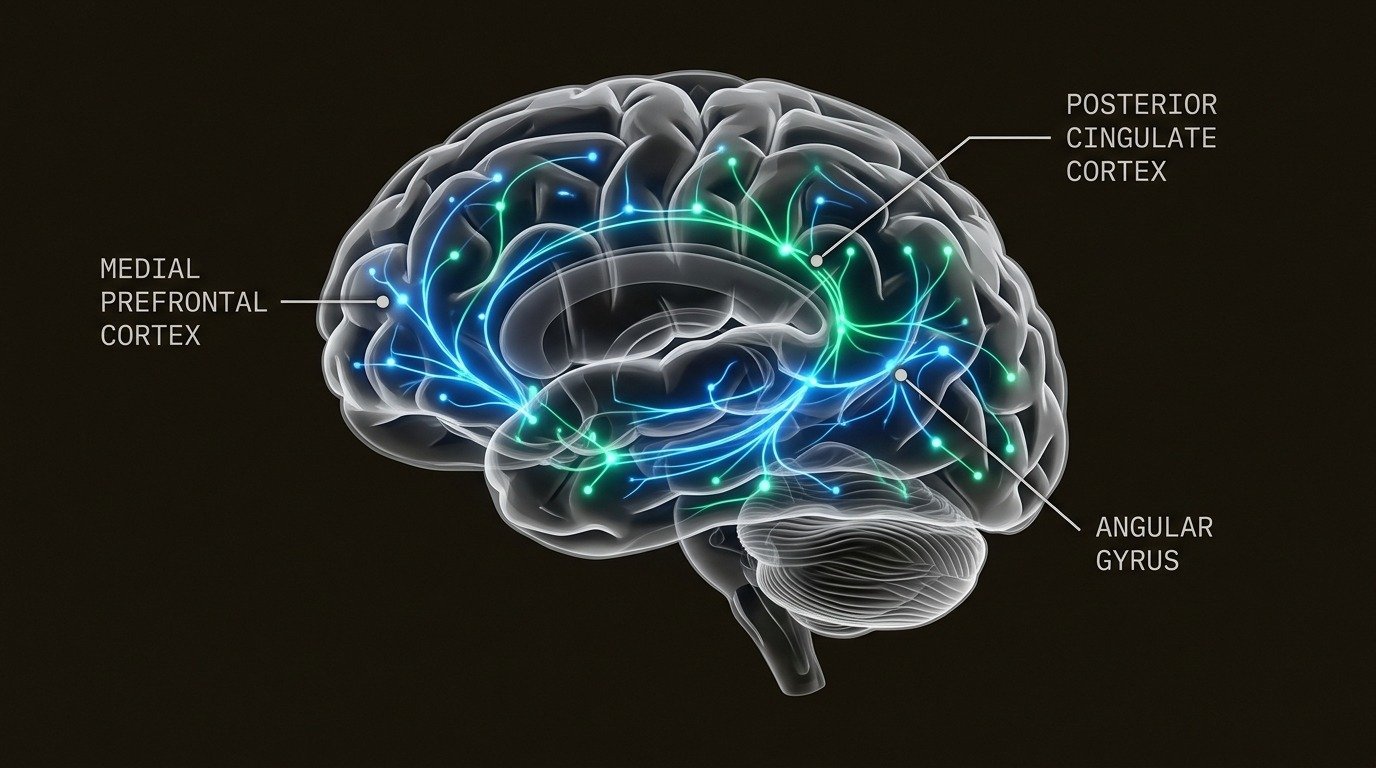
Usually, this wandering state is harmless. But for some people, the DMN becomes fixated on food. It gets co-opted by food cues, whether internal (a slight hunger pang) or external (seeing a food advertisement). This triggers what scientists call “food cue reactivity,” an evolutionary mechanism that once helped humans survive food scarcity. In modern environments saturated with food marketing and easily accessible high-calorie options, the mechanism becomes maladaptive.
One published review describes food noise as “maladaptive prospection”: your brain repeatedly simulates short-term reward scenarios (eating) that conflict with long-term goals (health and weight management). It is not that you lack discipline. Your brain’s default wiring has been hijacked by a constant stream of food-related thoughts. Interestingly, this phenomenon shares neural roots with conditions like depression, where the DMN also becomes overactive and generates repetitive thoughts.
GLP-1 medications quiet food noise by activating receptors in the brain’s appetite and reward centers, modulating the Default Mode Network, and dampening the dopamine response that food cues trigger. Synthetic GLP-1s mimic a hormone your gut naturally produces after eating, but they last much longer in your system, which means the signal they send to your brain is stronger and more sustained.
The mechanism works at three levels:
First, they act on appetite centers in the brain. GLP-1 receptors are found throughout the brain, including the hypothalamus (which regulates hunger), the hindbrain (which processes fullness signals), and the mesolimbic reward circuits that drive cravings. When activated, these receptors send powerful “I have had enough” signals to the rest of the brain. Research published in Diabetes, Obesity and Metabolism found that semaglutide significantly reduced appetite scores and food cravings by targeting these brain regions (Blundell et al., 2017).
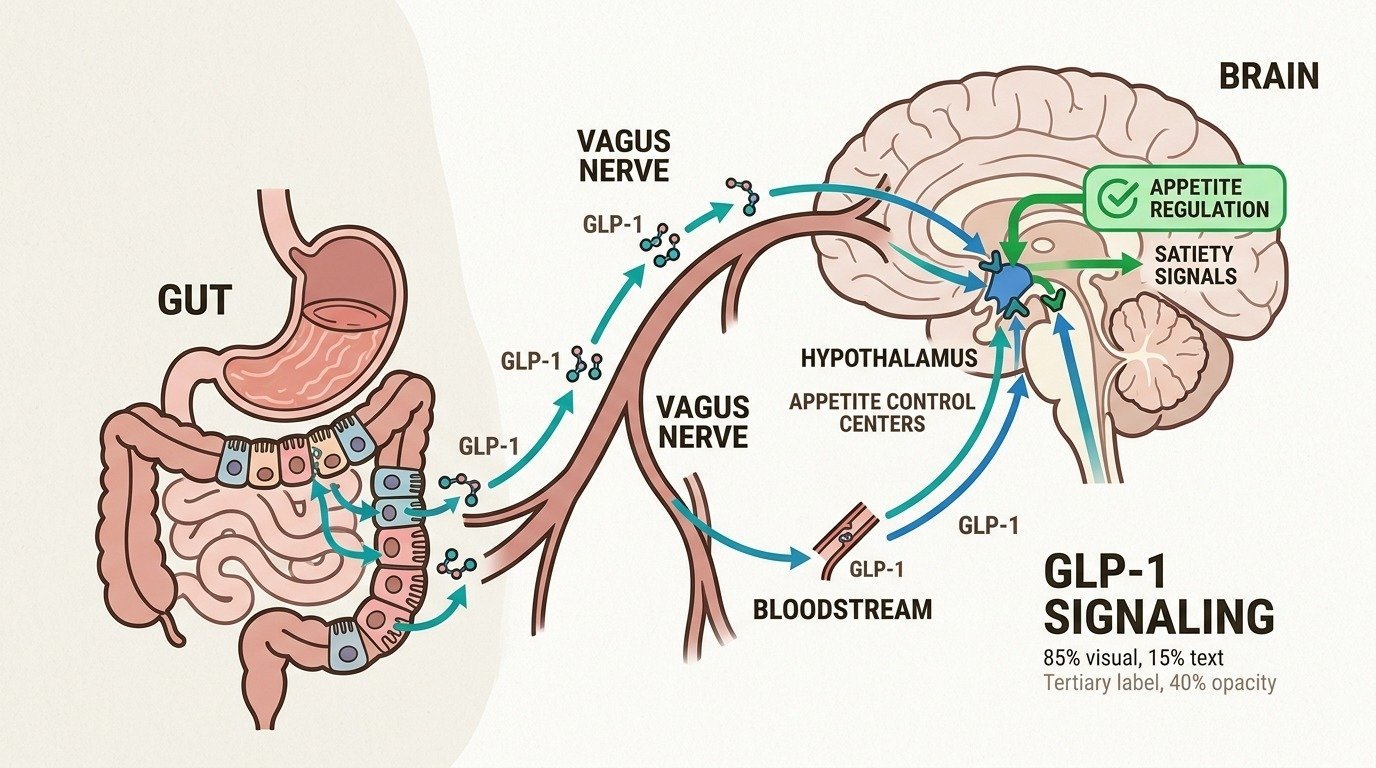
Second, they modulate the Default Mode Network. fMRI research shows that GLP-1 medications reduce DMN connectivity in regions associated with food-related rumination. This is the biological equivalent of turning down the volume on food noise.
Third, they alter reward processing. GLP-1s appear to reduce the dopamine response triggered by food cues. Importantly, patients still enjoy food, they simply stop obsessing over it. Researchers describe this as reducing the wanting without eliminating the liking. The natural gut-brain signaling pathway still carries fullness information through the vagus nerve; the medication amplifies and extends those signals so your brain gets a clearer, louder message about satiety that persists between meals. If you want the broader mechanism, see our primer on how GLP-1 medications work.
The evidence for GLP-1 medications reducing food noise goes beyond theory. A 2025 study presented at the European Association for the Study of Diabetes surveyed 550 people taking semaglutide for weight loss. The results were striking: before treatment, 62% of participants experienced constant thoughts about food throughout the day. After treatment, that number dropped to 16%.
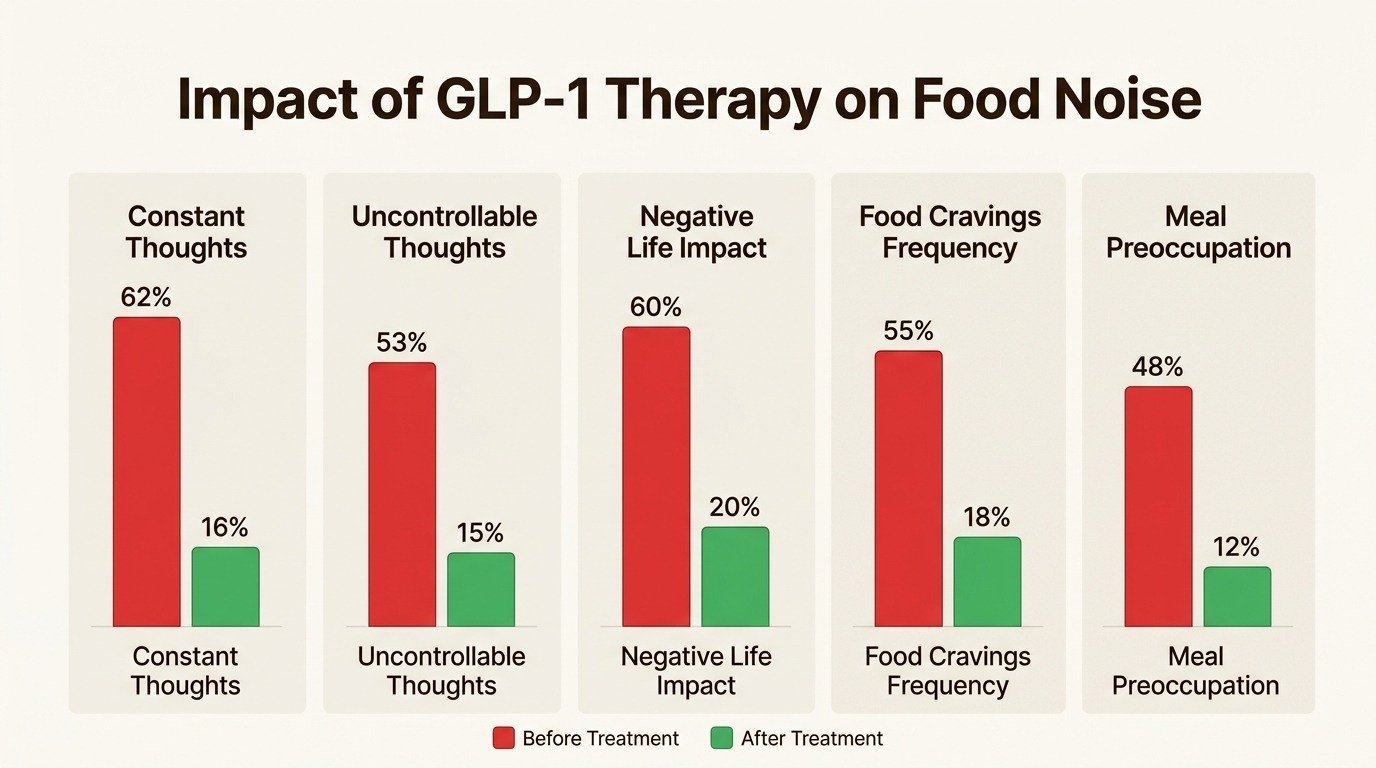
| Food Noise Metric | Before GLP-1 Treatment | After GLP-1 Treatment |
|---|---|---|
| Constant thoughts about food throughout the day | 62% | 16% |
| Spending too much time thinking about food | 63% | 15% |
| Uncontrollable food thoughts | 53% | 15% |
| Food thoughts distracting from daily activities | 47% | 15% |
| Negative effects on quality of life | 60% | 20% |
The mental health numbers were equally striking. Among the same participants, 64% reported improved mental health, 76% reported improved self-confidence, and 80% developed healthier habits. These effects appeared alongside the physical weight loss documented in the STEP 3 trial (Wadden et al., JAMA, 2021), which found that semaglutide combined with behavioral therapy produced 16% body weight loss with significantly improved control over eating.
Patients consistently describe the reduction of food noise as one of the most meaningful effects of GLP-1 treatment, often ranking it above the weight loss itself. The experience is not about feeling deprived or forcing yourself to eat less. It is about food simply occupying less mental space.
Common descriptions from Body Works patients include: “I can drive past a fast food restaurant without even noticing it,” “I eat dinner and actually feel done,” and “I did not realize how much mental energy I was spending on food until it stopped.” This mental freedom allows patients to redirect attention toward work, relationships, hobbies, and building sustainable habits alongside treatment. One patient interviewed in a widely read feature on food noise described it as “some part of my brain that was always there just went quiet. It felt almost surreal to put an injector against my leg and have happen in 48 hours what decades of intervention could not accomplish.”
According to the National Institute of Diabetes and Digestive and Kidney Diseases, GLP-1 medications are typically appropriate for adults with a body mass index (BMI) of 30 or higher, or adults with a BMI of 27 who also have weight-related conditions such as prediabetes, type 2 diabetes, high blood pressure, high cholesterol, or sleep apnea. Patients who describe persistent food preoccupation or repeated difficulty with appetite control and sustainable weight loss through diet and exercise alone tend to respond particularly well, because the medication targets the neurological driver of overeating rather than relying entirely on behavioral change.
Response varies from person to person. Some patients experience significant food noise reduction within days. For others, the effect builds more gradually as the dose is titrated upward over the first 16 to 20 weeks. Some patients experience mild gastrointestinal side effects during the early weeks, particularly during dose escalation. Working with experienced providers helps manage those effects while maximizing the benefit.
At Body Works, physicians in Franklin and Nolensville evaluate each patient individually through a comprehensive intake that includes bloodwork, health history, and body composition analysis. Your provider will determine whether semaglutide, tirzepatide, or another approach is the right fit. Schedule a Free Consultation to discuss whether GLP-1 therapy fits your situation.
Medically reviewed by Dr. Donald Vollmer, MD
Managing Physician, Body Works TN

If you have been struggling to lose weight despite trying diet after diet, you are not alone. For many people in Franklin, TN, Nolensville, TN,

Walking into a weight loss clinic for the first time stirs up a specific kind of anxiety. You have already tried diets, gyms, maybe even

Medical weight loss in Franklin and Nolensville, TN combines GLP-1 medications with physician supervision to address the hormonal and metabolic factors that make weight loss

If you are researching medical weight loss, two medication names keep coming up: semaglutide and tirzepatide. Both have changed what is possible with non-surgical weight

Everyone seems to know someone who dropped 20 pounds in a month on one of the new GLP-1 medications. The before-and-after photos are everywhere. The

Choosing between an in-person and online GLP-1 weight loss program is one of the most consequential decisions a patient can make before starting treatment. The