How IV Therapy Supports Autoimmune Disease Management
March 7, 2026
Living with an autoimmune disease often feels like your body has turned against you. One day you’re fine, and the next you’re dealing with crushing fatigue, joint pain, or brain fog that makes simple tasks feel impossible. Over 23.5 million Americans navigate this reality daily, searching for ways to manage symptoms and reclaim their quality of life.
While conventional treatments remain essential, many patients are exploring complementary approaches to support their overall wellness. IV therapy has emerged as one option that may help address specific challenges autoimmune patients face, particularly nutrient deficiencies and chronic inflammation. At Body Works, our licensed medical team works with patients to develop personalized treatment plans that integrate supportive therapies alongside conventional care.
Let’s explore what the research says about IV therapy for autoimmune conditions, how it works, and whether it might be right for you.
Understanding autoimmune diseases and your immune system
Your immune system is designed to protect you from harmful invaders like bacteria and viruses. But in autoimmune diseases, something goes wrong. Your immune system mistakenly identifies your own healthy cells as threats and launches an attack. The result? Chronic inflammation, tissue damage, and a wide range of symptoms that vary depending on which part of your body is being targeted.
Some of the most common autoimmune conditions include:
Rheumatoid arthritis attacks joints, causing pain and swelling
Lupus can affect skin, joints, kidneys, and other organs
Multiple sclerosis targets the protective covering of nerve cells
Hashimoto’s thyroiditis damages the thyroid gland
Crohn’s disease causes inflammation in the digestive tract
Celiac disease triggers immune response to gluten, damaging the small intestine
The symptoms often come in waves called flares. During a flare, you might experience extreme fatigue, joint stiffness, muscle aches, fever, and difficulty concentrating. Between flares, symptoms may subside, but the underlying condition remains.
Scientists still don’t fully understand what triggers autoimmune diseases. Genetics play a role, but environmental factors like infections, stress, and exposure to certain chemicals may also contribute. What we do know is that managing these conditions typically requires a multifaceted approach that addresses both the immune dysfunction and its downstream effects on your body.

What the research says about IVIG therapy
When discussing IV therapy and autoimmune diseases, it’s important to distinguish between two very different approaches. The first, and most thoroughly researched, is IVIG (Intravenous Immunoglobulin). This is a prescription medical treatment with FDA approval for specific autoimmune conditions.
IVIG consists of concentrated antibodies derived from the plasma of thousands of healthy donors. A comprehensive 2025 review published in Autoimmunity Reviews examined IVIG’s effectiveness across numerous autoimmune conditions. The researchers found consistent evidence supporting IVIG as a second-line treatment or adjuvant therapy capable of positively influencing the clinical course of many autoimmune pathologies while maintaining a good safety profile.
Currently, IVIG is FDA-approved for:
Kawasaki disease an inflammatory condition affecting blood vessels
Immune thrombocytopenia (ITP) low platelet count caused by immune destruction
Guillain-Barré syndrome a rapid-onset muscle weakness disorder
Chronic inflammatory demyelinating polyradiculoneuropathy (CIDP) progressive weakness and impaired sensory function
Multifocal motor neuropathy (MMN) progressive muscle weakness
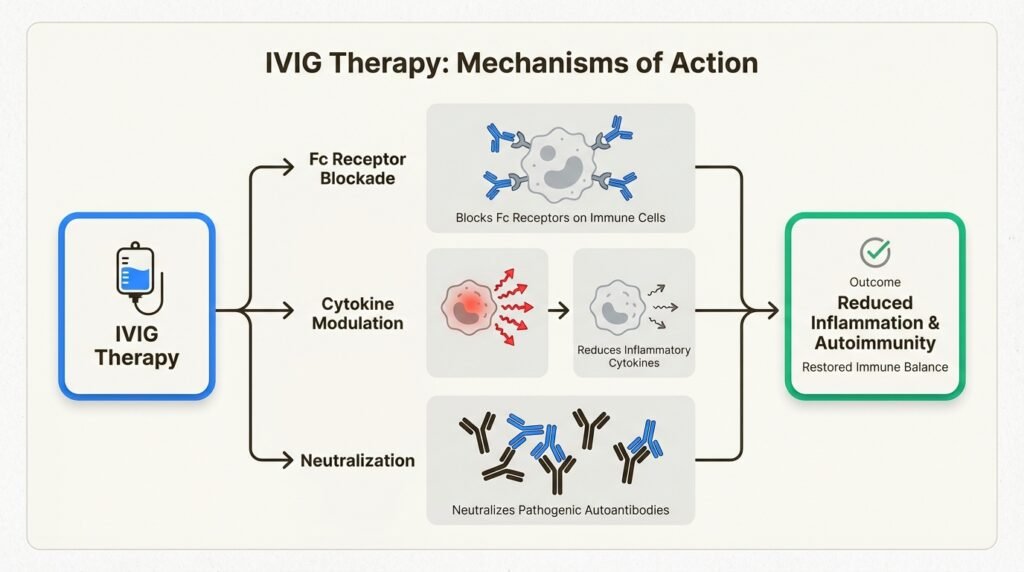
A 2023 study published in Antibodies detailed how IVIG works as an immunomodulator. The therapy appears to function through several mechanisms:
Fc receptor blockade prevents immune cells from attacking healthy tissue
Complement regulation reduces inflammation caused by the complement system
Cytokine modulation helps balance inflammatory and anti-inflammatory signals
Neutralization of pathogenic autoantibodies blocks the antibodies that attack your own cells
Research published in the Journal of Clinical Medicine suggests IVIG is often used off-label for conditions like myositis and vasculitis when conventional treatments prove insufficient. However, it’s important to understand that IVIG requires a prescription and is typically administered in clinical settings under medical supervision.
Nutritional IV therapy for autoimmune support
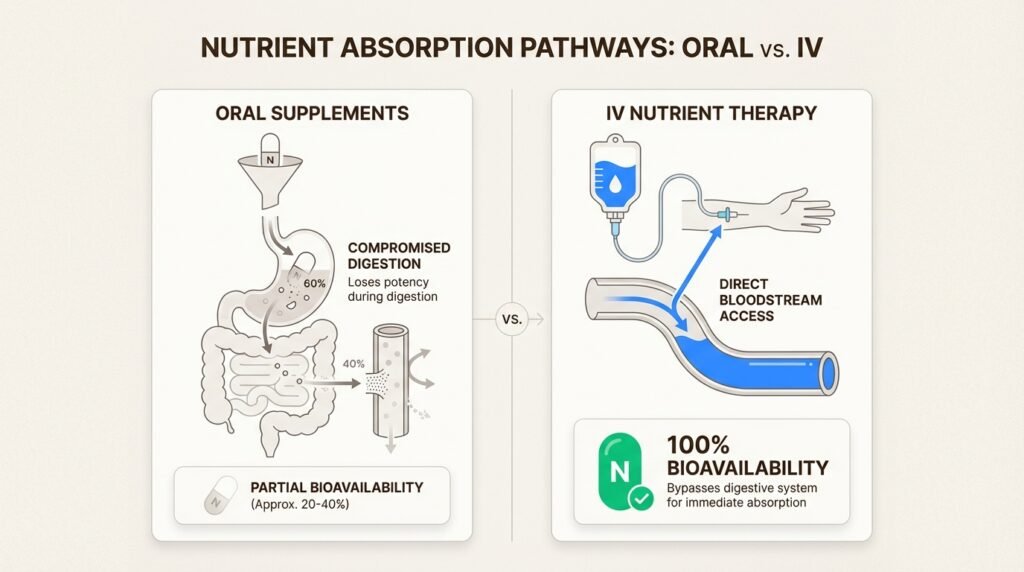
The second type of IV therapy takes a different approach. Rather than delivering immunoglobulins, nutritional IV therapy provides vitamins, minerals, and antioxidants directly into your bloodstream. This bypasses the digestive system entirely, which can be particularly beneficial for autoimmune patients who often struggle with nutrient malabsorption.
Why might this matter? Many autoimmune conditions affect the gut. Inflammatory bowel diseases like Crohn’s directly damage the intestinal lining. Even conditions that don’t primarily target the digestive system can cause inflammation that impairs nutrient absorption. When your gut isn’t absorbing nutrients effectively, oral supplements may not deliver the full benefit.
Common nutrients used in autoimmune-focused IV therapy include:
The Mayo Clinic offers a balanced perspective on this approach. Dr. Brent Bauer, director of research at Mayo Clinic’s Integrative Medicine and Health section, notes that while there’s limited evidence for IV vitamin therapy in people with normal nutritional levels, it can be effective for those with specific deficiencies or absorption issues. For autoimmune patients who struggle with malabsorption, this distinction matters.
It’s worth noting that nutritional IV therapy is not a cure for autoimmune diseases. Rather, it may help address specific symptom clusters like fatigue, inflammation, and nutrient deficiencies that often accompany these conditions.
Conditions that may benefit from IV therapy
While research continues to evolve, certain autoimmune conditions show particular promise for IV therapy support:
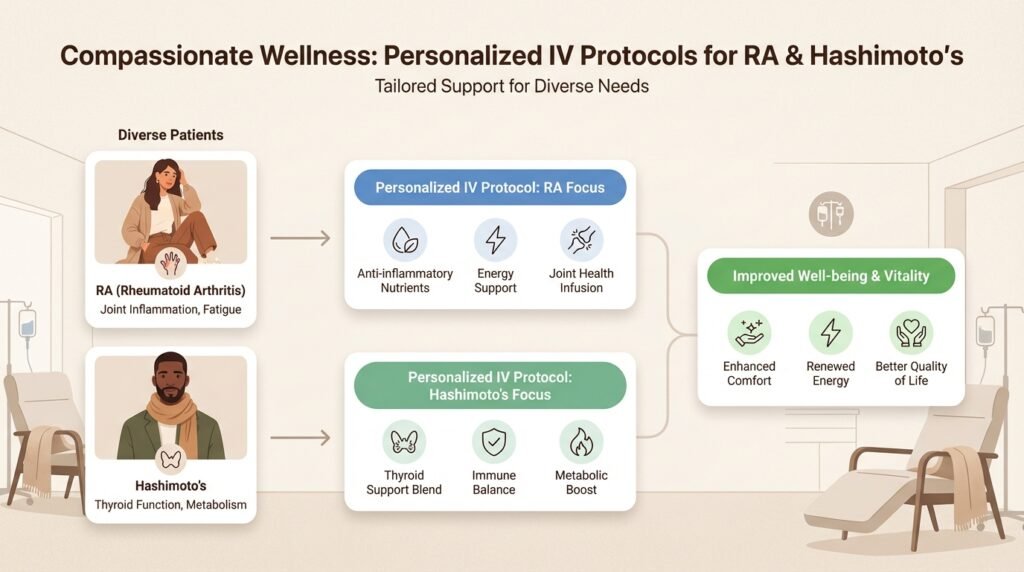
Rheumatoid arthritis patients may benefit from anti-inflammatory nutrients like vitamin C and glutathione. These compounds help combat the chronic inflammation that damages joints and causes pain.
Lupus often involves widespread inflammation and fatigue. IV therapy focused on hydration and immune-modulating nutrients may help support overall wellness during flares.
Multiple sclerosis affects the nervous system, making neuroprotective nutrients particularly relevant. Magnesium and B vitamins play crucial roles in nerve function and may offer supportive benefits.
Hashimoto’s thyroiditis patients frequently have specific nutrient needs. Selenium and zinc are essential for thyroid function, while B12 supports energy production that many Hashimoto’s patients struggle with.
Crohn’s disease and celiac disease both involve damage to the digestive tract that impairs nutrient absorption. IV therapy can deliver essential nutrients directly, bypassing the compromised digestive system entirely.
Chronic fatigue syndrome and fibromyalgia, while not strictly autoimmune, often overlap with autoimmune conditions and share symptoms like pain and exhaustion. Some small studies suggest IV nutrient therapy may help improve quality of life in these conditions.
The key point here is that IV therapy should complement, not replace, your conventional treatment plan. Medications prescribed by your rheumatologist or specialist remain essential for managing the underlying disease process. IV therapy may simply provide additional support for specific symptoms or deficiencies.
What to expect during IV therapy treatment
If you’re considering IV therapy, understanding the process can help you feel more comfortable. At Body Works, we prioritize making the experience as smooth as possible.
Your journey begins with a consultation. Our licensed Nurse Practitioners and Registered Nurses review your medical history, current symptoms, and any medications you’re taking. This helps us determine whether IV therapy is appropriate for your specific situation and design a personalized protocol.
The treatment itself is straightforward. You’ll relax in a comfortable chair while a small IV catheter is placed in your arm. The infusion typically takes 30 to 60 minutes, depending on the specific nutrients and your individual protocol. Many patients use this time to read, work on their phones, or simply rest.
Frequency varies based on your needs. Some patients start with weekly sessions and gradually extend the interval as their nutrient levels improve. Others find that monthly maintenance sessions work best for managing chronic symptoms. Your care team will work with you to find the right schedule.
What about results? Some benefits, like improved hydration, may be noticeable immediately. Others, such as reduced fatigue or decreased inflammation, typically develop over several sessions as nutrient levels in your body normalize. Most patients report feeling improvements within the first few weeks of treatment.
Side effects are generally mild and temporary. You might experience slight fatigue, a mild headache, or minor irritation at the IV insertion site. Serious complications are rare when treatment is administered by qualified medical professionals in a clinical setting.
You can learn more about our custom IV hydration services and how we tailor treatments to individual needs.
Is IV therapy right for you?
Deciding whether to incorporate IV therapy into your wellness routine requires honest assessment of your situation and goals.
Good candidates typically include:
Patients with documented nutrient deficiencies
Those experiencing significant fatigue or inflammation despite conventional treatment
Individuals with digestive conditions that impair nutrient absorption
People seeking complementary support alongside their existing medical care
However, IV therapy isn’t for everyone. It’s not a replacement for prescription medications that manage your underlying autoimmune condition. If you’re looking for a cure or hoping to stop your conventional treatments, IV therapy won’t meet those expectations.
Cost is another practical consideration. IV therapy typically isn’t covered by insurance when used for wellness purposes. At Body Works, we offer Cherry payment plans to help make treatment more accessible, with flexible monthly payments and no hard credit check.
Medical supervision matters. IV therapy should always be administered by qualified healthcare providers who understand autoimmune conditions and can monitor for potential interactions with your medications. Our team includes four Nurse Practitioners and three Registered Nurses who work under the direction of owner Justin Williams to ensure safe, personalized care.
If you’re curious about whether IV therapy might help you, the best next step is a conversation with our team. We offer free consultations at both our Franklin and Nolensville locations. During this consultation, we’ll discuss your health history, current symptoms, and whether IV therapy aligns with your wellness goals.
Living with an autoimmune disease is challenging, but you don’t have to navigate it alone. The right combination of conventional treatment and supportive therapies can help you feel more like yourself again. IV therapy represents one tool in a comprehensive approach to managing autoimmune conditions, and for many patients, it makes a meaningful difference in their daily quality of life.
Frequently Asked Questions
Medically reviewed by Dr. Donald Vollmer, MD
Managing Physician, Body Works TN
Browse Our Blog

Tirzepatide Deep Dive: Dosing, Results, and What Patients Should Expect
Tirzepatide is the newer of the two leading weight loss medications, and over the past two years it has been quietly displacing semaglutide as the
GLP-1 Weight Loss for Women in Menopause and Perimenopause: What Changes and What Helps
The weight gain that arrives during perimenopause is genuinely different from weight gain at other times of life. It often shows up around the midsection

Compounded Semaglutide: What to Look For, What to Avoid, and Why the Source Matters
For most of 2023 and 2024, semaglutide was on the FDA shortage list. That single regulatory designation opened the door for compounding pharmacies to legally

Semaglutide Results Timeline: Week-by-Week and Month-by-Month
The most common question patients ask after their first injection is some version of “when will I see results?” That question is reasonable, but the
GLP-1 Hair Loss: Why It Happens, How to Prevent It, and When It Grows Back
Hair shedding ranks consistently among the top concerns patients raise before starting semaglutide or tirzepatide. Search volume on “does semaglutide cause hair loss” has climbed
What Happens When You Stop Semaglutide or Tirzepatide: Rebound and Maintenance
Most patients on semaglutide or tirzepatide eventually ask the same two questions: how long do I need to take this, and what happens if I